- Benign Prostatic Hyperplasia
- Hormone Therapy
- Genomic Testing
- Next-Generation Imaging
- UTUC
- OAB and Incontinence
- Genitourinary Cancers
- Kidney Cancer
- Men's Health
- Pediatrics
- Female Urology
- Sexual Dysfunction
- Kidney Stones
- Urologic Surgery
- Bladder Cancer
- Benign Conditions
- Prostate Cancer
Making Sense of the Reintervention Rate for BPH
Partner Perspectives

During the virtual 2020 AUA annual meeting, it was proposed that perhaps “retreatment” has been reported differently and to different levels of detail in myriad BPH clinical trials.The call for consensus on definitions, new analysis techniques and reporting methods was further promoted in recent editorials and modeling work.1,2 This harkens back to the late nineties when Clavien proposed his classification for general surgery complications, later modified by Dindo and validated in 2004.3 Clavien and Dindo sought to reduce bias and improve understanding of surgical outcomes by explicitly classifying any “adverse deviation from normal postoperative course.”Perhaps antithetical to Clavien’s aim, however, the recent call to action in BPH focuses on schemes to bundle disparate events that are important to informing treatment decisions – surgical retreatment for failure to cure, treatment of complications, and possibly LUTS medication usage – into a single number by which we may compare treatment options, the “reintervention rate.” The proposed reintervention rate is blind to the invasiveness of procedure, as a TURP counts the same as a Prostatic Urethral Lift (PUL), an implant removal in the office, a urethrotomy, a fulguration for bleeding, and possibly even just continuing on Flomax. This confusing definition would reduce our ability to clearly communicate risk to patients, as these different types of events vary in importance dependent on the patient who is undergoing the procedure. Also, inherent to a “reintervention rate” are the assumptions that a steady recurring annual reintervention rate actually exists, and this rate is a good indicator for the durability of treatment effect. The question at hand is whether a new single metric of reintervention rate – rather than a detailed reporting of retreatment and Clavien-Dindo rated adverse events – will help us or indeed hurt us in our understanding of BPH treatments and our ability to reach the best shared decisions for our patients’ BPH care.
What are the “reintervention rates” for the leading BPH treatments?
Miller et al. calculate the annual reintervention rate by adding select interventions post treatment and dividing the sum by a uniquely modified “mean follow up” purportedly using life table analysis: Mean Follow-Up = Longest Follow-Up x (No. available patients at final follow up) / (No. patients enrolled). While there is no precedent for this methodology in BPH, the goal was to apply a statistical penalty to study results in an attempt to address the fact that most BPH trials lose about 20% of patients by 5 years for various reasons. Unfortunately, the authors applied the novel methodology to only one treatment option - Prostatic Urethral Lift (PUL). Repeating the method for other treatments puts the results into context (Table 1). The unexpectedly high number found for steam injection (RezumTM) is largely associated with treatment of post-operative retention by conducting CPT 53855 (placement of a urethral stent) followed later by CPT 52310 (retrieval of foreign body), the same code filed for PUL implant removal, the procedure Miller et al. included in PUL reintervention. The trends are, however, opposite. While the first PUL trials had a high rate of implant removal (9% patients requiring removal of a misdeployed implant), training has mitigated this problem with more recent studies showing 0% to <1% occurrence in over 1,400 patients.4,5 For steam injection, however, the randomized study patients had Foley catheters in place for an average of 3-4 days, but later real-world studies showed widespread usage of temporary stents, in addition to standard catheterization, as a way to mitigate possible irritative symptoms or even postoperative retention. It may be, however, that temporary stent usage will decrease in the future as the presence of necrotic tissue and a foreign body has led to infection rates as high as 23% in patients.6
Table 1: CALCULATED ANNUAL REINTERVENTION RATES
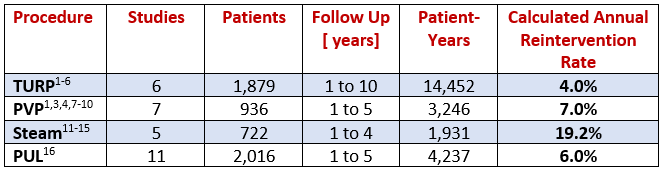
SOURCES:1. Bachmann A. J Urol 2015; 193(2): 570-8; 2. Varkarakis J. The Prostate 2004; 58: 248-251; 3. Lukacs B. Eur Urol 2012; 61: 1165-1173; 4. Capitan C. Eur Urol 2011; 60: 734-739; 5. Hill B. J Urol 2004: 171: 2336-2340; 6. Liu Z. Urol 2017; 103: 198-203; 7. Gu X. J Endourol 2011; 25(6): 1037-1041; 8. Guo S. J Endourol 2015; 29(4): 449-454; 9. Hai M. Urology 2009; 73: 807-810; 10. Malde S. J Endourol 2012; 26(7): 878-883; 11. Mooney R. Urol Pract 2020; 7(1): 28-33; 12. Dixon CM. Res Rep Urol 2016: 8: 207-216; 13. Greear G. J Urol 2020; 203(4S): e1280,PD61-02; 14. McVary KT. Urology 2019; 126: 171-179;15. Darson MF. Res Rep Urol 2017; 9: 159-168; 16. Miller LE. J Urol 2020 May 12
What we might consider definitive surgery, TURP and PVP laser show a relatively modest annual reintervention rate of 4%-7% per year. However, if we think about this further, this would mean we should counsel our BPH patient that, over the next 10 years, he will have a 40%-70% chance of needing a procedure if he chooses the gold standard treatment. This would be a very difficult message to receive and certainly would negatively bias the patient away from an intervention. Alternatively, we can counsel our patients as we do today, that they have about a 10%-20% chance of needing another TURP over the next decade and there is a 2%-7% risk of stricture or bladder neck contracture, 2%-3% risk of stress urinary incontinence, 7%-10% risk of erectile issues, and they will have a high probability of losing ejaculatory function (AUA Guideline on the Management of BPH, 2003). It would appear that this greater detail, as opposed to an overall reintervention rate, might be more helpful to patients in their decision making.
The main reason for the wide discrepancy between these two approaches to talking to a patient about risk lies in the assumption that there is, indeed, an annually recurring reintervention rate. Retreatment for failure to cure is generally more concentrated in the first year or two post-procedure, as seen in publications detailed in the recently updated AUA BPH Guidelines. PUL retreatment in the L.I.F.T. study was 4% in year 1, reducing to 3% in year 2 and to 0% in year 5.7 The GOLIATH study showed retreatment for PVP and TURP to be 3% and 1% in year 1, respectively, and 1% for both treatments in year 2.8 Similarly, treatment of complications is more likely in the first years. While 2.2% of TURP patients require treatment of bladder neck contracture in the first year, this high percentage of patients do not require this treatment every year. If we were to erroneously apply a recurring rate assumption, this would lead to an 11% reintervention rate for TURP at 5 years from this complication alone! Clinical studies and real world experience with TURP, PVP, PUL and Steam have shown that the assumption of a steady and recurring reintervention rate is a flawed concept that can predict much higher than observed episodes of reintervention.
How should we assess treatment durability?
Loss to follow up is a real concern in BPH clinical trials. The recent FDA draft guideline on BPH clinical trials states that loss to follow up should be kept below 20% over the course of the study (FDA, July 12, 2020). Unlike an oncology patient who is generally compelled to adhere to regular follow up, a BPH patient who feels better may perceive little reason to return, and one who feels worse may actively pursue care elsewhere. Within the “cloud” of loss to follow up, how should we interpret BPH treatment durability?
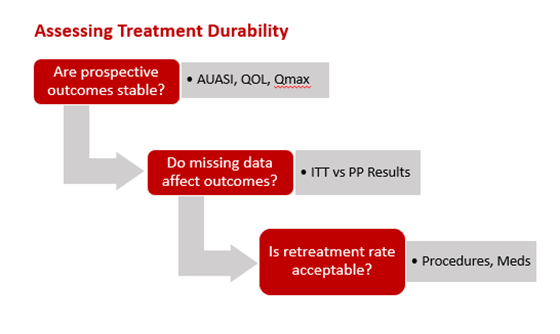
Intent to Treat analysis of data is standard in pharmaceutical trials but rare in longer term BPH procedure trials. It is valuable because it tests the effect of unavailable data on the reported means. Missing patients are scored based on their last available follow up or through an imputed value, as described in the FDA guideline. This result can then be compared to those typically reported (Per Protocol: using only available patients) to see if the absence of these patients might have inflated the reported outcomes. A landmark in BPH trials was the L.I.F.T. study in that the final 5 year PUL results were indeed analyzed and reported in this way; per protocol results were compared to the intent to treat results showing no significant effect from missing data. One hopes and expects that the publications on BPH devices in the future, including the 5 year results of the Rezum II study, will include this important analysis.
A question long asked in the urology community is whether use of BPH medications, both continued and de novo, constitutes retreatment. While this debate may continue, at a minimum, ongoing medication usage should be specifically reported in clinical publications. This has not been the case in the BPH literature and sufficient detail is rarely reported. For this reason, it is indeed premature to compare medication retreatment rates associated with BPH procedures. For instance, while the TURP randomized dataset is largely devoid of medication details, population studies show a trend. A recent study of the Canadian healthcare system included 58,038 men, followed for a median of 4.9 years after undergoing TURP. Surgical retreatment was 10.9% while continued use of LUTS medication was significant: 27% taking an alpha blocker, 20% 5ARI, and 15% an antimuscarinic medication.9 Is this very high rate of medication an indication that TURP is far less durable than we have understood it to be? Perhaps, instead, it suggests that patients may be electing prostate surgery too late in the disease process and residual, even irreversible bladder damage may have occurred. As new BPH treatments become less and less invasive, men may elect to address their obstruction earlier, effectively reducing the need for bladder medication thereafter. Shifting the BPH treatment paradigm forward with attractive minimally invasive options could, ironically, reduce overall population retreatment far more effectively than introducing more invasive procedures that many men avoid and defer until full bladder recovery is no longer possible.
A word of caution when comparing retreatment rates
When comparing low percentage rates, it is important to remember the requirement that a study be sufficiently powered to make any valid conclusion at all. For instance, in order to power a study to compare retreatment rates for PUL vs Steam at 5 years, using the original randomized trial results, 362 randomized patients would be required to achieve 80% power (alpha=.05).More recent study results (with less than one year of average follow up), which have reported a 5.8% PUL and 7.4% Steam retreatment rate , would require thousands of randomized patients to detect a difference.10 Clearly, this level of comparison is not available. It may be more appropriate to look at each treatment individually and determine if the retreatment is reasonable, given its safety and effectiveness profile, and beware of overzealous marketing claims of significant retreatment differences when data are limited by sample size.
How should we best assess safety and tolerability?
In what has been hailed a “renaissance in the care for patients with BPH” we are enjoying a growing list of minimally invasive surgical treatments (MISTs) for BPH patients.11 The Clavien-Dindo classification of adverse effects remains important, and should be consistently reported, to assure that new procedures are indeed less likely to cause such events and less invasive than traditional surgery. Any additional interventions should be specifically reported and classified. Importantly, adverse event rates must be reported per event category (e.g. anejaculation) and not potentially hidden in mean questionnaire scores (e.g. average MSHQ-EjD score). Clavien focused on morbidity of invasive surgery, but most goals for MIST lie almost exclusively in Clavien-Dindo I-II levels. As Kaplan describes, there is a need for a finer evaluation system to compare MIST options honestly and openly. This assessment focuses on patient goals of avoiding a postoperative catheter, returning to work and lifestyle within days, preserving all sexual function (including ejaculatory function), and being treated in the office setting. This last criterion may become even more important in this time of COVID.
Rather than calling for a single reintervention rate as a simplified treatment metric, we should perhaps turn our attention to consistent and detailed reporting of patient-centric adverse events and outcomes. Patients would greatly benefit from knowing these important details, which will likely lead to better shared decision making when choosing the best BPH treatment option.
References
1.McVary KT, Kaplan SA. A tower of Babel in today’s urology: disagreement in concepts and definitions of lower urinary tract symptoms/benign prostatic hyperplasia re-treatment. J Urol 2020; 204(2):213-214.
2.Miller LE, Stat P, Chugtai B, Dorbier RA, McVary KT. Surgical reintervention rate after prostatic urethral lift: systematic review and meta- analysis involving over 2,000 patients. J Urol 2020; doi: 10.1097/JU.0000000000001132.
3.Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of a 6336 patients and results of a survey. Ann Surg 2004; 240:205–213.
4.Eure G, Gange S, Walter P, et al. Real-World evidence of prostatic urethral lift confirms pivotal clinical study results: 2-Year outcomes of a retrospective multicenter study. J Endourol 2019;33(7):576-584.
5.Rukstalis D, Grier D, Stroup SP, et al. Prostatic urethral lift (PUL) for obstructive median lobes: 12 month results of the MedLift study. Prostate Cancer Prostatic Dis 2019;22(3):411-419.
6.Mollengarden D, Goldberg K, Wong D, Roehrborn C. Convective radiofrequency water vapor thermal therapy for benign prostatic hyperplasia: a single office experience. Prostatic Cancer Prost Dis 2018; 21(3):379-385.
7.Roehrborn CG, Rukstalis DB, Barkin J, et al. Five year results of the prospective randomized controlled prostatic urethral L.I.F.T. study. Can J Urol 2017; 24(3); 8802-8813.
8.Thomas JA, Tubaro A, Barber N, et al. A multicenter randomized noninferiority trial comparing GreenLight-XPS laser vaporization of the prostate and transurethral resection of the prostate for the treatment of benign prostatic obstruction: two-year outcomes of the GOLIATH study; Eur Urol 2016; 69:94-102).
9.Campbell J, Reid J, Ordon M, Welk B. The utilization of benign prostatic hyperplasia and bladder-related medications after a transurethral prostatectomy. Urology. 2019;130:126-131.
10.Greear G, DePina T, Bechis S. Retreatment for persistent lower urinary tract symptoms after convective water vapor thermal prostate ablation. J Urol 2020; 203(4S):e1280.
11.Kaplan SA. De-MISTifying less-invasive solutions for BPH. Urology Times®. 2019;47(9):22-26.
Funding/Support: This review and comparative analysis was sponsored by NeoTract Inc. | Teleflex. The sponsor played a role in the analysis and interpretation of the data and in preparation of the article.
Rezum is a trademark of Boston Scientific.
