Articles by Jeni Williams

Recent research shows contemporary imaging and biopsy techniques often fail to identify contralateral tumors in men presumed to have unilateral prostate cancer-and the results have significant implications for identifying candidates for hemiablation.

A study of kidney stone patients who were treated using ureteral access sheaths found no evidence of ureteral strictures an average of 4 years following ureteroscopy.

A multicenter study in the United Kingdom found 5-year prostate cancer control rates following treatment with focal therapy are similar to those of patients who have undergone radical prostatectomy, even when accounting for variation in tumor location, size, and risk.

Chronic opioid use is rare following radical prostatectomy in Europe. Slightly more than half of men undergoing RP in Sweden between 2007 and 2017 were found to have filled an opioid prescription, but the proportion who became chronic opioid users was less than 1%.
A new tool for kidney stone ablation demonstrates strong potential to dust and fragment stones more quickly and efficiently than devices currently available in the United States. However, clinical studies must be performed before this technology can be used during lithotripsy nationally.
Patients with kidney stones who rank their pain at the maximum level on a 100-point scale or whose number-one goal for treatment is to relieve pain are less likely to reach their treatment goals than other patients undergoing kidney stone treatment, a recent study found.

A recent study found low levels of free testosterone in older men with prostate cancer could increase these men’s odds of facing erectile dysfunction after undergoing radical prostatectomy.
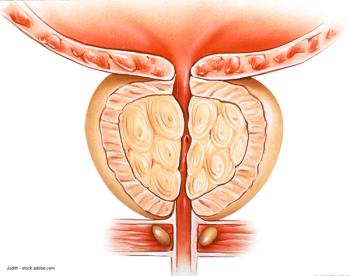
Urology Times interviewed four leading urologists who are experts in BPH to get their take on the most important BPH studies of 2018 and 2019.

A patient-reported outcomes survey that is widely used to determine whether men are experiencing erectile dysfunction (ED) fails to ask three critical questions that could uncover whether men truly have ED and the extent to which they face challenges, researchers say.

A study presented at the AUA annual meeting in Chicago shows higher rates of emergency department (ED) visits when ureteral access sheaths are used during ureteroscopy to remove kidney stones.

Forgotten stents are one of the most common challenges urologists and their patients face, and they can cause significant complications and increase costs of care. Now, a program that tracks stent insertion and removal in the electronic medical record shows strong potential to help eliminate retained stents.

High rates of residual fragments after ureteroscopy point to the need to both improve selection of patients for this procedure and find ways to boost stone-free rates, according to researchers at UT Southwestern Medical Center, Dallas.

As the number of patients who receive onabotulinumtoxinA (onabotA [Botox]) injections for overactive bladder increases, so does the age of this population and their associated comorbidities. This raises the question: Is the use of onabotA in patients who are taking anticoagulant or antiplatelet medication safe?

Three novel androgen receptor inhibitors provide an embarrassment of riches when it comes to treatment options for nmCRPC patients, but there are still questions to be answered-including the extent of these drugs’ clinical benefit.

A recent study shows older women with decreased levels of serum testosterone are more likely to experience incontinence, but this does not necessarily mean urologists should be giving testosterone to older women, a study author says.

Are dip tests needed for onabotulinumtoxinA (onabotA [Botox]) bladder procedures when no symptoms of urinary tract infection are present? A recent study presented at the AUA annual meeting in Chicago suggests the answer may be no.

A preliminary study of the use of salvage lymph node dissection in patients with nonmetastatic, castration-resistant prostate cancer indicates the potential to delay disease recurrence as well as the use of systemic therapies through this approach.

Researchers say the use of apalutamide (Erleada) in patients with high-risk, nonmetastatic castration-resistant prostate cancer improves metastasis-free survival in patients who have previously undergone radical prostatectomy or external radiotherapy-regardless of the type of treatment they received.

A survey of low-risk prostate cancer patients found men who choose active surveillance over definitive treatment have similar mental health outcomes.

Men with low levels of free testosterone 3 months after undergoing radical prostatectomy could face increased chance of early recurrence of prostate cancer, according to researchers from the University of California Irvine.

More research is needed to determine the value of using magnetic resonance imaging to predict pathology outcomes following radical prostatectomy, according to a study presented at the AUA annual meeting in Chicago.

























