- Vol 48 No 2
- Volume 48
- Issue 2
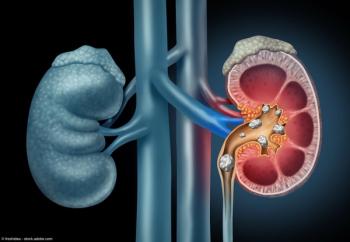
Stone management often falls short
Overcoming challenges of medical therapy starts with leveraging guidelines.


Kidney stones are common and are on the rise, according to government statistics. About 11% of U.S. men and 6% of women develop urolithiasis once or more during their lifetime, according to the National Institute of Diabetes and Digestive and Kidney Diseases. Recurrence is common, too-occurring at a rate of up to 50% within the first 5 years of the first stone episode, researchers reported in an article published Feb. 25, 2016 in Nature Reviews Disease Primers.
Despite the high prevalence of kidney stones and recent AUA guidelines to medically manage them, urologists don’t do a very good job at managing stone patients, according to Kyle Wood, MD, assistant professor of urology at University of Alabama at Birmingham.


“We’re very good at surgically treating stones, and we’ve had significant advancements within the surgical realm with equipment and lasers and optics,” Dr. Wood said. “But we’ve done a pretty poor job as a practice at managing kidney stones and advancing our field in regard to medical management. I think the biggest issue is we haven’t even followed our guidelines.”
Also see:
Brian R. Matlaga, MD, MPH, professor of urology and director of The Stephens Center for Stone Disease at Johns Hopkins University School of Medicine in Baltimore, said there is good evidence that medical therapy reduces future stone events. But the evaluation can be cumbersome, primarily from the patient’s standpoint.
“The 24-hour urine collection is a cumbersome type of a test to do,” Dr. Matlaga said. “The interpretation of it has become easier in recent years with commercial laboratories that provide some guidance for therapies based on reported lab results. But still it requires ultimately a urologist to prescribe medication and then follow the patient to assess how effective those medications are in reducing their risk factors.
“It brings the patient to a longer-term relationship with the physician than just someone that shows up, has a symptomatic stone, the stone is removed, and then the relationship is over.”
Another real-world challenge in medical stone management is the lack of innovation aimed at reducing stone risk.
“The medications we’re using today in 2020 are the same medications that were used 2 and 3 decades ago,” Dr. Matlaga said. (Also see,
Nevertheless, urologists can optimize the care they provide kidney stone patients by leveraging best practices in guideline documents, including the AUA’s Medical Management of Kidney Stones guideline, which Dr. Matlaga and other authors reviewed and updated in 2019.
The first evidence-based steps
Guideline first author Margaret S. Pearle, MD, PhD, vice chair of urology and professor of urology and internal medicine at UT Southwestern Medical Center in Dallas, said urologists first need to determine which stone patients need further evaluation.
“We really want to identify the high-risk patients,” she said. “We typically do a screening evaluation that consists basically of a careful history looking for any underlying conditions that are associated with stones, a family history of stones, any medications that are associated with stone production, and blood work. Blood work can identify some medical conditions like renal tubular acidosis or primary hyperparathyroidism that are associated with recurrent stones.”
Dr. Wood said research at University of Alabama suggests about 7% of the kidney stone population has primary hyperparathyroidism and about one-fourth of those patients are misdiagnosed or not diagnosed by the providers who referred them to the academic center.


If the history and blood work fail to uncover any risk factors in a patient who has had only one stone, Dr. Pearle said she makes general dietary recommendations but doesn’t do full metabolic testing. She does recommend full metabolic testing, including one, preferably two, 24-hour urine tests and blood work for patients who have recurrent stones or risk factors in their history.
Read:
“In those patients in whom we obtain a 24-hour urine, we look at all the parameters-total volume, pH, calcium, oxalate, uric acid, citrate, sodium-the important parameters of the urine that give us indications of underlying causes. We make recommendations based on those results,” Dr. Pearle said. “Some abnormalities can be managed with dietary measures, some require medication, and often it’s a combination of both.”
Next -
Controversies muddy kidney stone medical management. One is the importance of the 24-hour urine collection, which helps to guide stone treatment and management, experts say.
Also see -
“One of the essential things to do is a 24-hour urine-in my opinion, ideally two 24-hour urines. Yet, if you look at the data nationally, probably less than 10% of our stone formers are getting the appropriate metabolic workup,” Dr. Wood said.
It’s one thing to order the test; it’s another to have patients complete it correctly for accurate results.
“In reality, if we’re going to be ordering the 24-hour urine, we have to be willing to spend time with patients to discuss accuracy and compliance,” Dr. Wood said. “We recently published an article [in Urology Practice, Jan. 1, 2019] looking at our compliance rates. Even though we order the test, our compliance rate was only about 50%, meaning half the people weren’t performing the studies that we were ordering.”
Dr. Wood said a slight change during the study brought up the compliance rate.
“We basically did the paperwork for our patients so they would get the 24-hour urine kit sent to their houses. That increased our compliance from 47% to 65%,” he said.
Dr. Wood and colleagues also published an examination of the accuracy of the 24-hour urine test in stone formers (Rev Urol 2018; 20: 119–24). That study found that even though patients receive the kits, many don’t use them properly. One solution is patient education, including time spent with patients, handouts, and take-home instructions.
Medical management best practices
Dietary recommendations are an important part of the medical management of stone disease, but the approach shouldn’t be cookie cutter, according to the experts interviewed for this article.
“Volume is probably the single most commonly recommended dietary change-just increasing fluid intake. That’s primarily because the more dilute the urine, the lower the concentration of the minerals, the less driving force there is for stone formation,” Dr. Pearle said.
Dr. Matlaga said the goal is to achieve a urine volume of about 2 liters a day by drinking at least 2 liters of fluids daily. Some of his patients are using wearable devices help them accomplish the task.
“For example, there are now smart water bottles that can link to smartphones, and they can help make sure patients consume their target fluid consumption,” Dr. Matlaga said. “I think we’re starting to see the use of technology helping support some of these dietary and lifestyle changes.”
There are, however, controversies around which fluids, other than water, are best. Findings of some epidemiologic studies are at odds with small metabolic studies looking at various fluids, according to Dr. Pearle.
Large cohort epidemiologic studies, she said, suggest coffee, tea, beer, wine, and orange juice are associated with reduced risk for first-time stone formation, while sugar-sweetened beverages are associated with an increased risk. A randomized trial looking at the effect of soft drinks found an increased risk of stones with soft drink consumption based primarily on phosphoric acid-based soft drinks rather than citric acid-based soft drinks (J Clin Epidemiol 1992; 45:911-6). Metabolic studies examining fruit juice consumption have found orange juice consistently shows a benefit in stone formers because it provides alkali in the form of potassium citrate.
“There is a lot of controversy about lemonade, despite general interest in the the community for lemonade consumption as a stone prevention measure. There have been metabolic studies that have not shown a benefit of lemonade. People have looked at other juices as well with mixed results,” Dr. Pearle said.
Generally recommended dietary measures for kidney stone patients include maintaining a normal calcium intake and limiting salt intake and animal protein.
While the value of limiting animal protein is controversial, metabolic studies have shown that animal protein is a risk factor for stone formation because it increases urinary uric acid. Uric acid binds to inhibitors of stone formation, reducing inhibitory activity in the urine. Animal protein also provides an acid load, which lowers urinary citrate and urine pH, according to Dr. Pearle.
“Despite mixed evidence, we generally recommend limiting animal protein intake to no more than two servings a day,” she said.
In patients with low citrate in urine, Dr. Pearle recommends increasing fruits and vegetables, which are high in alkali. Alkali drives citrate into the urine.
Oxalate restriction is highly controversial among urologists.
“There is strong data to support a significantly increased risk of kidney stones in people with increased oxalate and increased urinary oxalate excretion. The biggest issue is there is a lack of good data on what foods to restrict and what foods to avoid,” Dr. Wood said.
Research to date suggests patients who are high in oxalate should avoid spinach and potatoes. Dr. Wood also recommends patients refer to the Harvard database of dietary oxalate content for other foods high in oxalate (
Oxalate restriction in patients who don’t have an oxalate problem might not be necessary, according to Dr. Wood. Urologists can confirm whether oxalate is a driver of a patient’s stone disease with a 24-hour urine collection.
Dr. Pearle said she recommends at least modest restriction of foods high in oxalate, but it’s a balance if those foods are part of an otherwise healthy diet.
Read:
“Things like nuts and whole grains, beans, beets, and potatoes are all high in oxalate, so a lot of people who are healthy eaters can have very high urinary oxalate. If the oxalate is very high, it is reasonable to recommend being careful about oxalate intake, but at least from my standpoint, in patients with a normal urinary oxalate, I don’t generally focus on oxalate too much,” Dr. Pearle said.
Next:
Thiazides remain the mainstay of kidney stone treatment for hypercalciuria that is not secondary to high salt intake, according to Dr. Wood.
While important, thiazide treatment is likely underused because it requires that urologists follow up with labs. Thiazides, according to Dr. Wood, also treat hypertension and can interact with other anti-hypertensive medication.
“Patients with aggressive stone formation and high urinary calcium who have normal urinary sodium and are consuming normal amounts of or the recommended daily allowance of calcium would benefit from thiazide diuretics that lower urinary calcium,” Dr. Pearle said.
The evidence also suggests potassium citrate or other alkalization methods effectively manage kidney stone disease, according to Dr. Wood.
Also see:
“Those, too, are usually directed by the 24-hour urine or sometimes by stone compositions,” he said.
Again, there are barriers to treatment. Potassium citrate, or UroCit-K, can be extremely expensive and difficult for patients to tolerate, as gastrointestinal side effects are common, according to Dr. Wood. Another issue with potassium citrate is the need to monitor patients who may have chronic kidney disease with labs to make sure they don’t become hyperkalemic while on the medication.
One medication that urologists shouldn’t be using as a first-line treatment for uric acid stones is allopurinol, according to the AUA guideline.
“The key to prevention of uric acid stones is not to lower urinary uric acid but to raise pH. Allopurinol is occasionally indicated if patients still form stones despite correcting urine pH, but they will likely continue to make stones on allopurinol if you don’t correct pH,” Dr. Pearle said.
We want to hear from you! What are some best practices you use when managing stones? Email us at
Articles in this issue
almost 6 years ago
Bladder cancer biomarker test accurately adjudicates atypical cytologyalmost 6 years ago
TP-Bx: The answer to rising infectious complications?almost 6 years ago
The case for transperineal prostate biopsy vs. the transrectal approachalmost 6 years ago
Can you afford to avoid MIPS participation?almost 6 years ago
What are Category III codes, and how are they best used for billing?almost 6 years ago
Study compares prostate cancer treatment functional outcomesalmost 6 years ago
PSMA-targeted therapy well tolerated in men with mCRPCalmost 6 years ago
Risk of chronic opioid use low after RPalmost 6 years ago
Trial supports combined behavioral, medical approach to treating OABNewsletter
Stay current with the latest urology news and practice-changing insights — sign up now for the essential updates every urologist needs.